This is a demonstration of the use of advanced approaches to synthetic biology in medicine, although we will need a lot of improvements before such a system is actually usable to treat humans. The main credit for this achievement goes to Anže Smole, a young Slovenian researcher who is now in the USA taking post-doctoral training at the University of Pennsylvania, where he is researching immunotherapy for cancer in one of the leading groups in this field. We hope that in a few years he will bring his wealth of experience back to Slovenia. It would be nice if until then we could take advantage of our knowledge, and in cooperation with physicians start treating Slovenian patients with lymphomas through immunotherapy.

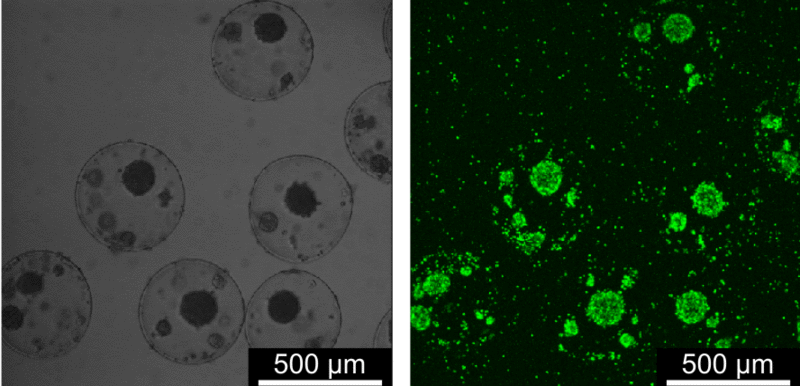
The group of Slovenian scientists created the prototype of a cellular device that is inserted into the organism, and then functions automatically as a prosthetic organ. Staff of the Department of Synthetic Biology and Immunology at the Institute report that they have modified human cells so that they can independently recognise inflammation processes in the body and begin producing and secreting anti-inflammatory proteins as treatment. This involves cellular therapy, where capsules containing modified cells are placed in the body, and they begin secreting therapeutic proteins only when inflammation occurs. The cells are protected in porous capsules against their own immune system, so the same type of cell can be used for all patients, which could increase the accessibility of cellular treatment. Through the porous capsules the cells can receive nutrition, and upon activation they secrete therapeutic proteins such as antibodies that neutralise inflammation, in a similar way to biological medicines for the treatment of inflammatory intestinal diseases. The cellular device therefore spends most of the time waiting and sensing in the body, checking on the state of any inflammation. It is triggered automatically if inflammation occurs, and then begins secreting the medication.
Staff at the Institute of Chemistry staff say that the cells can detect inflammation even before the patient or doctor are aware of it, and this is particularly important in reducing the negative effects of such events. Researchers have tested the system on cell cultures and in pre-clinical trials on an animal model of inflammatory intestinal disease, and the results show that if the capsules containing cells are placed inside the stomach cavity then they can prevent injury to the intestines.
"This is a demonstration of the use of advanced approaches to synthetic biology in medicine, although we will need a lot of improvements before such a system is actually usable to treat humans. The main credit for this achievement goes to Anže Smole, a young Slovenian researcher who is now in the USA taking post-doctoral training at the University of Pennsylvania, where he is researching immunotherapy for cancer in one of the leading groups in this field. We hope that in a few years he will bring his wealth of experience back to Slovenia. It would be nice if until then we could take advantage of our knowledge, and in cooperation with physicians start treating Slovenian patients with lymphomas through immunotherapy," said Roman Jerala, who headed the project.
What is involved in this work?
The conceptual basis for the research was set out by Dr. Anže Smole in his doctoral thesis under the mentorship of Roman Jerala, while Duško Lainšček, Urban Bezeljak and Simon Horvat were co-authors. As Smole said for the Multimedia Centre of RTV Slovenia, "this involves engineering mammal cells, which we deliberately modify by teaching them to perform new or additional functions, which we can use for therapeutic purposes."
The research itself lasted four years, since it involves very complex matters. Producing modified cells required the coordination of individual modules, ranging from the sensor that detects inflammation, to the amplifier of the combination of therapeutic proteins and other experiments, including modelling. The most important contribution for this last part came from Urban Bezeljak, who is currently pursuing a doctorate at the famed Institute of Science and Technology (IST) in Austria.
A paper entitled A Synthetic Mammalian Therapeutic Gene Circuit for Sensing and Suppressing Inflammation by authors Anže Smole, Duško Lainšček, Urban Bezeljak, Simon Horvat and Roman Jerala was published in the January edition of the distinguished scientific journal Molecular Therapy.
What does this discovery mean for the treatment of diseases?
As Jerala explains, "this achievement represents a prototype for a cellular device for treating inflammatory as well as other diseases, where we used cells to function as diagnostic media and as an autonomous smart device for local production and dosing of medication. Cellular therapy is in fact still in its infancy, and for the moment significantly less modified cells are used, for instance, to treat cancer. Undoubtedly, though, with this approach we have shown the possibilities for the future development of treatment."
Currently there is no realistic possibility for the discovery or device they used in the research project to become an actual clinical treatment. "We would need to make stable cells and carry out a range of safety tests before human use. It is, however, highly probably that similar cellular devices will start to be used in clinical medicine in the coming decades," added Jerala.
Polona Prešeren, Sinfo
This is a demonstration of the use of advanced approaches to synthetic biology in medicine, although we will need a lot of improvements before such a system is actually usable to treat humans. The main credit for this achievement goes to Anže Smole, a young Slovenian researcher who is now in the USA taking post-doctoral training at the University of Pennsylvania, where he is researching immunotherapy for cancer in one of the leading groups in this field. We hope that in a few years he will bring his wealth of experience back to Slovenia. It would be nice if until then we could take advantage of our knowledge, and in cooperation with physicians start treating Slovenian patients with lymphomas through immunotherapy.